- 49
- 148
December 14, 2022
Nanchong City, Sichuan Province
The 31-year-old woman reportedly suffocated to her death outside of Gaoping No. 5 Hospital after being denied entry because she was suffering from a high fever. She died moments after the video was shot. The hospital claimed that the cause of death was “acute myocarditis.”
- 65
- 532
It's truly unbelievable how more angles and footage are STILL being released after 20+ years!
- 38
- 135
A man is filmed agonizing on the floor of his bedroom by his wife after she poisoned him with what appears to be strychnine, judging by how he twitches throughout the whole video.
- 25
- 129
Music credits
Epic Sport Racing Car | DRIVE by Alex-Productions | https://onsound.eu
Music promoted by https://www.free-stock-music.com
Creative Commons / Attribution 3.0 Unported License (CC BY 3.0)
https://creativecommons.org/licenses/by/3.0/deed.en_US
Sad Piano by Alex-Productions | https://onsound.eu
Music promoted by https://www.free-stock-music.com
Creative Commons / Attribution 3.0 Unported License (CC BY 3.0)
https://creativecommons.org/licenses/by/3.0/deed.en_US
!MOMENTO_MORI
- 54
- 366
Demons Call by BatchBug | https://soundcloud.com/batchbuMusic promoted by https://www.free-stock-music.com
Creative Commons / Attribution 3.0 Unported License (CC BY 3.0)
- 71
- 218
Pomf2 copy
Video I saved in the mid 2000's.
Has ogrish and divX watermarks.
Original auto was corrupted so I had to change it.
Music by:
CURSE by Mehul ShaRma | https://instagram.com/mehul_sharmaofficial/
Music promoted by https://www.free-stock-music.com
Creative Commons / Attribution 3.0 Unported License (CC BY 3.0)
https://creativecommons.org/licenses/by/3.0/deed.en_US
Remastered for image quality by:
Rainonthescarecrow
- 75
- 150
On a Monday afternoon in February 2020, 42 year old Sarah Boone called police to report that she’d found her boyfriend, 42 year old Jorge Torres Jr, dead in a suitcase.
She claimed that on the previous evening they had been drinking wine, doing puzzles, and playing hide and seek when she convinced Jorge to climb into the suitcase, but after, she says, she fell asleep by mistake.
Sarah’s account would be contradicted by a video police found on her phone which showed her taunting Jorge while he struggled to breath inside the suitcase.
Witnesses claimed that it wasn’t unusual to hear Sarah and Jorge fighting, and both had been previously arrested for assaulting one another.
In 2018, Sarah was arrested for strangling Jorge, who claimed he had to fight her off to avoid dying. Sarah said it happened because Jorge hit her in the eye for talking to another man.
Jorge’s autopsy suggested he had suffocated inside the suitcase for 11 hours.
He had cuts and bruises all over his body.
Sarah Boone was charged with second-degree murder. Her trial is set to begin in November, 2022.
- 87
- 259
Maggots are fucking gross they make my stomach turn, I'd rather piss shards of broken glass than to be infested with maggots.... Myiasis is the subject of the first installment of a new project im working on called 'Nightmare Fuel'.
We will see how this one goes and if people like it I'll make more, if people don't like then I wont.
maggot gif
heres some more videos of people infested with maggots
Case reports
41 years old female resident in Brazil, with history of psychiatric disorders, who lived with her 73 year old father and her husband, a known alcoholic with history of physical violence to both father-in-law and wife.
She suffered a knife injury to the 2nd finger of the left hand, and was not able to seek immediate medical care; instead a handkerchief was used to control the bleeding and cover the wound. Six months after, neighbours were warned by a strong odour emitting from the finger, and took the patient to seek medical care.
She was presented to the Emergency Department (ED) with a large area of finger necrosis and amputation, associated with cellulitis extending from the finger's base to the hand; at naked eye, one could observe the live larvae infesting the healthy tissue in drilled pocket-like holes under the skin (Fig. 1). In face of such an advanced lesion, asphyxiation or pharmacologic treatment alone would not suffice, and prompt treatment was conducted – broad-spectrum antibiotics and tetanic prophylaxis were initiated, and she was submitted to extended surgical resection (metacarpophalangeal disarticulation) and mechanical removal of 132 live larvae. Entomological study (morphological study) determined it to be Cochliomyia hominivorax (Diptera: Calliphoridae) – New World Screworm (NWS) – larvae. Besides infestation treatment, the socio-economic problems were identified and conducted to the proper social services.
A 52-year-old man presented with bilateral foot pain worsening on the left preventing him from ambulating. He recalled developing frostbite of all ten toes 4-5 months prior to admission, when at that time, he was admitted to a local hospital and underwent right transmetatarsal amputation but did not follow-up with his wound care. The patient was homeless and dwelled in shelters and abandoned houses. He reported developing erythema, tenderness and swelling of his left foot; however, he did not seek medical attention because he otherwise felt “ok.” He reported seeing maggots on the left foot but stated that “the maggots are fine, they are cleaning it out.” He denied fever, chills, nausea, vomiting, or lightheadedness. On physical examination, the patient's vital signs were normal except for mild tachycardia, which immediately resolved with one bolus of intravenous normal saline. His left foot (Figures 1 and 2) revealed severe skin ulceration extending to the mid-foot, exposing all phalangeal bones, and many colonies of maggots. There was surrounding erythema, swelling, tenderness and malodor, but otherwise clean margins with no necrotic tissue or purulence. Left peripheral pulses were normal at the dorsal pedis. Laboratory tests revealed no leukocytosis, lactic acidosis, and negative serial blood cultures. Imaging revealed acute on chronic osteomyelitis of left foot. The patient underwent an uncomplicated left below knee amputation and revision of previous right transmetatarsal amputation. He was discharged to rehabilitation but has not adhered to outpatient wound follow-up.
An 80 years-old female patient was brought to Accident & Emergency Department of a hospital in southern Poland by ambulance, presenting with a large ulcerative lesion covering most of the right side of her face and the nose. The wound was approximately 15x12 cm and encompassed the right eye socket with missing eye bulb; one could see moving maggots surrounded by liquefied tissues. The patient was in poor general status, not able to move and with very little mental contact, severely dehydrated with yellowish skin colour and visibly malnourished and hygienically neglected
The patient was found by accident during a police intervention in a flat inhabited by her alcoholic son. By accounts of her son, she was recently bedridden and an ulcerating lesion on her face was possibly noted many months before. There was no medical care sought and the sanitary conditions in the living quarters were very poor.
A 60-year-old male, smoker, and alcoholic patient with OSCC, who refused initial cancer treatment and sought hospital care with an extensive facial lesion and approximately 150 larvae in the extraoral region. The treatment was given through the administration of 6 mg of Ivermectin associated with the surgical removal of the larvae. Subsequently, palliative chemotherapy began.
44-year-old man diagnosed with invasive oral squamous cell carcinoma. The treatment consisted of manual removal of the larvae and cleaning with aqueous chlorhexidin. The patient's management was antisepsis, larval removal, and general care, performed weekly. The patient died 2 months later.
After a minor motor vehicle accident, police brought a 75-year-old man to the emergency room because he was observed to have a large cranial lesion. Examination revealed a 15 x 17 cm frontal bone defect with eroded frontal dura, exposed cortex, and massive cortical maggot infestation.
The patient was empirically treated with intravenous antibiotics for meningitis. Maggots (Phaenicia sericata, or the green bottle fly) were removed by suction, attrition, and gentle contact exposure to a mild bleach solution. Biopsy of the scalp and cranium revealed angiosarcoma, for which operative treatment was refused. The patient was transferred to a skilled nursing facility for palliative care where he died 3 months later.
43-year old homeless alcoholic male had gangrene of the scrotum and penis, urethro-cutaneous urinary fistula with numerous live and motile larvae on the surfaces. In both patients, some larvae were removed and sent to the lab for identification. The larvae were identified as maggots of the fly Luciliasericata. Antibiotic therapy, disinfection, and debridement with sterile covering of the wound were used. RESULTS For both patients, complex treatment of myiasis was successful, and patient recovered without parasitic consequences
Patient 73 years old, born in São Paulo. He reported an ulcerated lesion on the penis for eight months with progression in size during the period and also local pain and left inguinal nodulation. The main comorbidities were diabetes mellitus, hypertension, varicose ulcers in both lower limbs and obesity. There was no family history of neoplastic disease. The patient underwent incisional biopsy of the penile lesion. The diagnosis was invasive squamous cell carcinoma
After chest X-ray and computed tomography of the abdomen and pelvis, he was clinically staged as EcT2cN2M0. The proposal was partial amputation of the penis. While the patient waited to be called for surgery, he presented himself at the emergency room, with local bleeding and larvae emerging from the lesion. On the same date, he underwent treatment of penile squamous cell carcinoma and myiasis through partial penectomy
The anatomopathological report showed a squamous cell carcinoma of 6.0 × 4.4 × 3.3 cm, moderately differentiated infiltrating the glans, foreskin and balanoprepucial groove. Absence of infiltration of the cavernous and spongy body. There were free surgical margins. He evolved without dehiscence or infection of the postoperative wound, being discharged on the second postoperative day and receiving an outpatient orientation after antimicrobial treatment with clindamycin for ten days for scheduling bilateral inguinal lymphadenectomy
a 67-year-old homeless woman with hearing impairment who is living in extremely poor sanitary conditions and was taken by a friend to the gynecology service of a public hospital from Cali, Colombia. The patient presented with a clinical picture of undetermined onset, consisting of ulcerated lesions in the vulvar region, tenderness, and multiple larvae coming out of her vagina (Figure 1). Obstetric and gynecologic history was unknown. On physical examination, she had an edematous vulva, with multiple live maggots in the vulvar vestibule. After initial extraction of maggots, necrotic tissue, edema, friable tissue, and erythema was evident in the vulvar region and introitus.
She was admitted to the hospital for management and for investigation. She was initially evaluated by the gynecology team, and direct examination revealed multiple larvae in the vulvar vestibule and introitus. She was also evaluated by a multidisciplinary team, including clinical nutrition and psychiatry and was tested for other infections. During her stay, she was diagnosed with HIV, syphilis, and schizophrenia.
Although several larvae were extracted, no specimen was sent for larval species identification. Identifying the species may not change the treatment but is important to understand the epidemiology of local urogenital myiasis. It has been recommended that at least one maggot should be sent to the laboratory for identification of the species for epidemiologic purposes
An 85-year-old female patient was admitted to the Department of Ophthalmology, Dicle University Faculty of Medicine, with the complaint of a wound in her right eye for over 1 year. Larvae had been in the same eye for 1 week. The patient had a history of an acne-like lesion for 7 years in her lower eyelid, which had been excised 2 years previously in another clinic. One year after excision it had recurred in the same region. Despite all our attempts, we could not obtain the documents on the patient's initial surgery.
The clinical examination showed no light perception in her right eye; the eyelid was thickened and there was a necrotic, loose tissue lesion 3×4 cm in diameter, invading inferiorly into the upper side of the maxilla, superiorly to the roof of the orbita, medially to the lateral part of the nose, and laterally to the ossa zygomatica (Figure 1).The conjunctiva was hyperemic, the cornea was cloudy, the iris was normal, pupils were normal, and light responses were absent. There was a cataract in the lens of the right eye and the fundus could not be examined.
Light-sensitive and motile larvae were detected in the lesion. With forceps, 71 larvae were extracted from the lesion within 48 hours (Figure 2). The larvae had 12 segments and were 8–15 mm in length. By parasitological examination, it was determined that the larvae were in the third developmental phase of Hypoderma bovis, a member of the Oestridae family.
Visual acuity in the patient's left eye was 2/200 and intraocular pressure was 15 mm Hg. Anterior segment findings were normal except for an inferiorly dislocated lens with cataract. By ultrasound, both globes were evaluated as normal. A 3×4 cm-diameter solid mass with heterogeneous density filled the right maxillary sinus, and superiorly reached the nasal bone and medial rectus muscle. The impaired bone structure in the right eye was detected by computed tomography (CT). No escaped larvae were detected in the CT scan. The ocular bulbus, retrobulbar space, extraocular muscles and optic nerve were normal in the left eye. No intracranial invasion was found by CT. No metastasis was detected in other examinations.
Orbital exenteration, total maxillectomy and graft repair were conducted in the right eye. Pathological examination confirmed basal cell carcinoma. During the six-month period of follow-up, orbital tomography and clinical examinations were performed, and the patient was examined and evaluated for recurrence and metastasis.
Music
Witch By The Sea by Darren-Curtis | https://soundcloud.com/desperate-measurez
Music promoted by https://www.free-stock-music.com
Creative Commons / Attribution 3.0 Unported License (CC BY 3.0)
https://creativecommons.org/licenses/by/3.0/deed.en_US
Flesh And Bones by BatchBug | https://soundcloud.com/batchbug
Music promoted by https://www.free-stock-music.com
Dark Trap | DARKNESS by Alex-Productions | https://onsound.eu/
Music promoted by https://www.free-stock-music.com
Creative Commons / Attribution 3.0 Unported License (CC BY 3.0)
https://creativecommons.org/licenses/by/3.0/deed.en_US
BLACK FLY by Audionautix | https://audionautix.com
Music promoted by https://www.free-stock-music.com
Creative Commons / Attribution-ShareAlike 3.0 Unported (CC BY-SA 3.0)
https://creativecommons.org/licenses/by-sa/3.0/deed.en_US
Like Tears in the Rain by Adam Matejko | https://soundcloud.com/adam-matejko-698390533
Music promoted by https://www.free-stock-music.com
Creative Commons / Attribution 3.0 Unported License (CC BY 3.0)
https://creativecommons.org/licenses/by/3.0/deed.en_US
Demons Call by BatchBug | https://soundcloud.com/batchbuMusic promoted by https://www.free-stock-music.com
Creative Commons / Attribution 3.0 Unported License (CC BY 3.0)
https://creativecommons.org/licenses/by/3.0/deed.en_US
Bonus
There is a HIDDEN Marsey somewhere in the video, the first user to posts a screen shot of the hidden Marsey in the comments will win 1,000 Mbux..
If the winner is also a member of
!Memento_mori or a follower I'll double the prize and give them 2,000.
if the winner is a member and a follower I'll give them 3,000 Mbux!
Note: the marsey at the end of the video is NOT the hidden Marsey
Now there is more to find and more to win!
Along with Marsey I've add 5 more hidden WPD related things for you to find each one will be worth 500 coins or mbux (which ever I have at the time) and each prize will be increased to 750 if the winner is a !Memento_mori member and to 1000 if the winner is also a follower!
the 5 new characters to look for are in the pictur below.
sources
https://www.ncbi.nlm.nih.gov/pmc/articles/PMC6074300/
https://www.sciencedirect.com/science/article/abs/pii/S1067251613001944
https://www.sciencedirect.com/science/article/pii/S187603411730014X
https://shmabstracts.org/abstract/worked-to-the-bone-a-severe-unusual-case-of-wound-myiasis/
https://www.sciencedirect.com/science/article/pii/S2210261220303151
https://www.wjomi.com/article2.html
https://pubmed.ncbi.nlm.nih.gov/17621006/
https://www.sciencedirect.com/science/article/pii/S187603411730014X
https://www.sciencedirect.com/science/article/pii/S2214442020302990
https://www.sciencedirect.com/science/article/pii/S1201971222003563
https://www.ncbi.nlm.nih.gov/pmc/articles/PMC3255963/
https://www.sciencedirect.com/science/article/abs/pii/S0021515503000777
https://shmabstracts.org/abstract/worked-to-the-bone-a-severe-unusual-case-of-wound-myiasis/
- 48
- 203
All recent 13 episodes of "Now You Fucked Up!", edited together with seamless transitions.
All the credit for the creative-editing go to "mindspun" of Kaotic.com
My "72 Dumb Ways To Die" MEGA-COMPILATION can be found here: https://watchpeopledie.tv/h/misc/post/8914/72-dumb-ways-to-die-megacompilation
- 101
- 197
Video info and credits
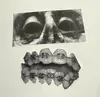
The specimens seen in this video are all apart of the Naguib Pasha Mahfouz collection which are housed at the Naguib Pasha Mahfouz museum in Egypt. These are the first specimens in this collection to be digitally photographed and uploaded to the internet as part of what is going to be the museum's digital platform & venue once finished.
Music
The title and artist of the song in the beginning is unknown to me.
Lair by Lucas King
https://youtube.com/@LucasKingPiano
Demons call by BatchBug
sound mixed and edited by Rainonthescarecrow
Embryonic and Fetus Anatomical Fluid-Preserved Specimens
Other terms used:
Wet Specimens
Fetal Specimens
Miscarriage Specimens
Stillborn Specimens
Pickled Punks (Carney and sideshow term)
Purpose:
Medical study, and research
Public education
Carnival/Sideshow/Freakshow Exhibits
Legacy:
Embryonic and Fetus Specimens were instrumental to our understanding of early life development, pregnancy, and child birth.
Were vital to the development of the medical fields of Obstetrics and Gynaecology.
The knowledge gained from studying these specimens has led to treatments, procedures, and extremely important insights that have saved countless lives.
About Naguib Pasha Mahfouz
Professor Mahfouz is looked upon as the father of Obstetrics and Gynaecology in Egypt. He was the first professor of the speciality in Egypt and the Middle East. He established the first midwifery school in Egypt. His book on obstetrics “The Art of Midwifery and Obstetrics” remains a classic until this day. He established the first clinic for the neonates in Cairo in 1927 and the government adopted the scheme nationwide after the success of the first clinic.
Naguib Mahfouz qualified in 1902. He volunteered to work in a town in Asyiut, where an epidemic of cholera had just broken out. He traced the source of infection to a polluted water well that supplied most of the town with water. After condemning the well, the epidemic came to an end. He set his heart on specialising in obstetrics and gynaecology. He had his personal reasons because his own delivery was a complex one as his mother was in obstructed labour for three days. He was recommended by the British General Health Manager of Egypt to join Qasr el Eini Medical School where he was appointed assistant surgeon. He then established the first outpatient gynaecological clinic in Egypt. It proved to be very popular. The medical school appointed him as the first professor of obstetrics and gynaecology in the country.
He pioneered surgery of gynaecologic fistulae, his work on fistulae remains a standard operative technique until this day. A copy of his book, “Mahfouz Atlas Of Gynaecology and Obstetrics” is kept in the library of The Royal of Obstetricians and Gynaecologists in London.
He established the first pathology museum in gynaecology which was highly commended by the President of the Royal College of Obstetricians and Gynaecologists of the day.
The Nobel prize winner Nagib Mahfouz the writer was named after Professor Mahfouz.
A freezing day on 5 January 1882. “I was born in a state of white asphyxia, the worst form of foetal distress. I was breathless when I was born and did not meet life with screams as most babies do. The midwife and doctor who attended my mother took me for dead. I was placed, together with the placenta, in a copper tray near an open window. My family was told that I was stillborn. Half an hour later my aunt Hana whispered to the midwife that she noticed that the baby was breathing feebly every few minutes whereupon the midwife wrapped me up, cut the cord, and did what she could to resuscitate me.”
From such a precarious start to life, Naguib Mahfouz went on to become the first Egyptian professor of obstetrics and gynaecology at Kasr-El-Aini Hospital, a post he occupied until he retired in 1947. Among his many achievements, his research into surgical techniques of fistula repair made him world famous. He was a prolific author on a wide variety of subjects including urinary and faecal fistulas, fibroids, ectopic pregnancy, ovarian tumours, pelvic infections, and endometriosis.
The Mahfouz museum at Kasr-El-Aini Hospital, which he founded at his own expense, contains a unique collection of obstetric and gynaecological specimens. His magnum opus, the Atlas of Mahfouz's Obstetrics and Gynaecological Museum (John Sherratt, 1949), was described by the then president of the Royal College of Obstetricians and Gynaecologists, Sir Eardley Holland, as “no doubt the best book that has appeared in obstetrics and gynaecology.” Mahfouz became a fellow of the Royal College of Physicians and an honorary fellow of the Royal College of Obstetricians and Gynaecologists, the Royal College of Surgeons of England, and the Royal Society of Medicine.
In his autobiography (The Life of an Egyptian Doctor, Livingstone, 1966) Mahfouz tells why he specialised in obstetrics and gynaecology: “One day . . . Dr Shoukry . . . asked me to help him in a difficult case of labour. I went with him to his clinic and there found on the operating table a lady whom they had tried, unsuccessfully, to deliver with forceps without anaesthesia. For two hours Dr Shoukry tried, unsuccessfully, to deliver the head with forceps but it would not come down. He then asked me to change places with him and try to do a podalic version and bring down a foot as my hand and arm were thinner than his. I declined saying that I had no experience whatsoever in deliveries. Dr Shoukry tried to pull down a foot and it took him a whole hour before he succeeded. He and his assistant were able to deliver the body of the foetus up to the shoulders only but the head would not come down. They went on pulling the shoulders until the body of the foetus was severed from the head. I suggested taking the patient to the Government hospital or else calling an obstetric surgeon into consultation. They replied that among all the Egyptian and foreign doctors in Alexandria there was not one who was an Obstetrician. In the morning . . . I was told that she (the patient) had died during the night with the baby's head still in her uterus. . . . It was then that I resolved to do everything in my power to study obstetrics and gynaecology and to dedicate my life to help women suffering from difficult labour.”
Naguib Mahfouz was initially assigned to the Cairo railway station to examine suspected cholera patients coming from Upper Egypt. Not a man who would shy away from the call of duty, Mahfouz paid a visit to the Health Department Director General and demanded to be sent to Mousha, a village in Upper Egypt near Assiut which was particularly hard-hit by the deadly disease and where a doctor had just succumbed to the same disease he had been sent to fight. A bewildered Director General could only agree to his request. In Mousha, Young Mahfouz traced the cholera deaths to an infected well in a farmer's house. Within a week of the discovery of the well, the Mousha cholera epidemic had come to an end. It is ironic that a nineteen-year-old medical student succeeded where a body of the ablest and most experienced British Public Health Department experts had failed. Mahfouz subsequently had similar success in fighting cholera in each of Deirout in Upper Egypt and Alexandria.
Naguib Mahfouz qualified as a doctor in December 1902 coming top of his year. In 1904 and after a two-year spell at Suez hospital, he was appointed as an anaesthetist at Kasr El Aini hospital. As there was no such thing as a department of obstetrics or gynaecology at Kasr El Aini hospital, Mahfouz started a weekly gynaecological outpatient clinic. This turned out to be such a success that two whole wards were soon dedicated to obstetrical and gynaecological patients. This is how the first department of obstetrics and gynaecology in Egypt came into existence. Much of the experience that Mahfouz acquired in dealing with difficult labour came from an agreement that he had struck with the medical officers who delivered women at home. Whenever these were faced with a difficult labour, they would call him into attendance. For his part, he would attend to the patient's house and help them deal with the most complicated cases at no fee whatsoever for himself. During the subsequent fifteen years, Mahfouz attended about two thousand women with difficult labour in their own homes. During this time, he recalls sleeping no more than two nights a week in the comfort of his own home. One of the children that Naguib Mahfouz delivered, after a difficult labour, was named after him in 1911. This child later became the Laureate of the Nobel prize in literature, the famous novelist Naguib Mahfouz.
Naguib Mahfouz was appointed as Professor of Obstetrics and Gynaecology at Kasr El Aini Medical School in January 1929, a post he occupied until he reached the age of retirement in January 1942. His term of service at Kasr El Aini was extended by five years at the unanimous request of his colleagues at the department of Obstetrics and Gynaecology. Mahfouz was also obstetrician and gynaecologist to the Egyptian Royal Family. His pioneering work on the surgical repair of urinary and faecal fistulae brought him and Kasr El Aini hospital international acclaim. Such was his reputation that the leading lights in his speciality came all the way to Egypt to watch him repair fistulae at Kasr El Aini and the Coptic Hospitals. Such was his fame and international acclaim that he was invited to lecture and show films of his operations at the Universities of London, Oxford, Edinburgh, Geneva and Lausanne, to name a few.
A great handicap to Naguib Mahfouz's work was the absence of a maternity unit at Kasr El Aini hospital. Thanks to his efforts and unrelenting campaigning, the first maternity centre in Egypt came into existence at Kasr El Aini. Mahfouz reorganised the School of Nursing and Midwifery and taught general nursing and midwifery to its pupils for over thirty years. No less than one thousand midwives graduated under him. His two books on nursing and midwifery were used by the students for many years. In 1919, he started a pioneering scheme whereby midwives, trained to the highest standards by himself, were allowed to deliver women in their own homes. It is interesting to note that a similar scheme was only started a year later in England. In 1919, Mahfouz introduced, for the first time in Egypt, antenatal clinics at the Kasr El Aini maternity hospital as well as in the centres that he had opened in Cairo's deprived areas. Following this, he established a child welfare section at Kasr El Aini hospital, the first of its kind in Egypt. Many mother and child welfare centres were then built throughout the country.
The Collection
By 1930, Naguib Mahfouz had managed to collect three thousand of the rarest specimens in obstetrics and gynaecology obtained from his operations. That same year, he offered the museum which housed them and which was named after him, as a gift to the Kasr El Aini Medical School. The Naguib Mahfouz Museum of Obstetrics and Gynaecology still exists to date at Kasr El Aini Medical School. In 1945, the museum was described by the then President of the Royal College of Obstetricians and Gynaecologists of England, Sir Eardley Holland, as “a remarkable collection” and ” a wonderful monument to the name of its founder”. Mahfouz provided specimens to the museums of each of the universities of Ein Shams, Alexandria, Assiut and Khartoum.
sources:
https://en.wikipedia.org/wiki/Naguib_Pasha_Mahfouz
https://copticmedical.com/dr-nagib-mahfouz/
https://www.nourelrefai.com/gallery/Naguib-Pacha-Mahfouz-Museum/
https://pubmed.ncbi.nlm.nih.gov/35099840/
Bonus
There is a HIDDEN Marsey somewhere in the video, the first user to posts a screen shot of the hidden Marsey in the comments will win 1,000 Mbux..
If the winner is also a member of
!Memento_mori or a follower I'll double the prize and give them 2,000.
if the winner is a member and a follower I'll give them 3,000 Mbux!
Note: the marsey at the end of the video is NOT the hidden Marsey
- 56
- 154
In China, a girl decided to poison her boyfriend due to a relationship dispute in a college. The boy died instantly.
- 50
- 116
As you can see, this turmeric party is a thing here in India where relatives of the groom apply turmeric to the groom signifying happiness in the married life of the couple but you never know when and where the Angel of Death is waiting for you and when it comes, it doesn't wait. This video reminds me of a verse from Quran
حَتَّىٰٓ إِذَا جَآءَ أَحَدَهُمُ ٱلْمَوْتُ قَالَ رَبِّ ٱرْجِعُونِ ٩٩
Until, when death comes to one of them, he says, 'My Lord, send me back, that I might do righteousness in that which I left behind.' No! It is only a word he is saying; and behind them is a barrier until the Day they are resurrected." (Surah Al-Mu'minun 23:99-100)
— Dr. Mustafa Khattab, the Clear Quran


















 (elderly man has a heart attack while making sex)
(elderly man has a heart attack while making sex)













.webp?x=8)
](/images/16613348824524522.webp)
](/images/16613348825883472.webp)










](/images/1663338632635266.webp)
















 Slavshit
Slavshit

 Sandshit
Sandshit
